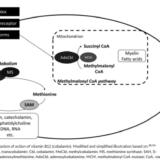
Description:
According to a newly published cohort study in JAMA Neurology on August 11, 2025, men with dementia have a 24% higher risk of mortality and greater healthcare utilization—particularly hospitalizations—compared to women with the same condition (1).
Main Content:
Dementia is rapidly increasing worldwide in both sexes, with an estimated 55 million people currently living with the condition and nearly 10 million new cases each year, posing a substantial burden on healthcare systems and society (2). Gender differences may partly contribute to disparities in dementia outcomes.
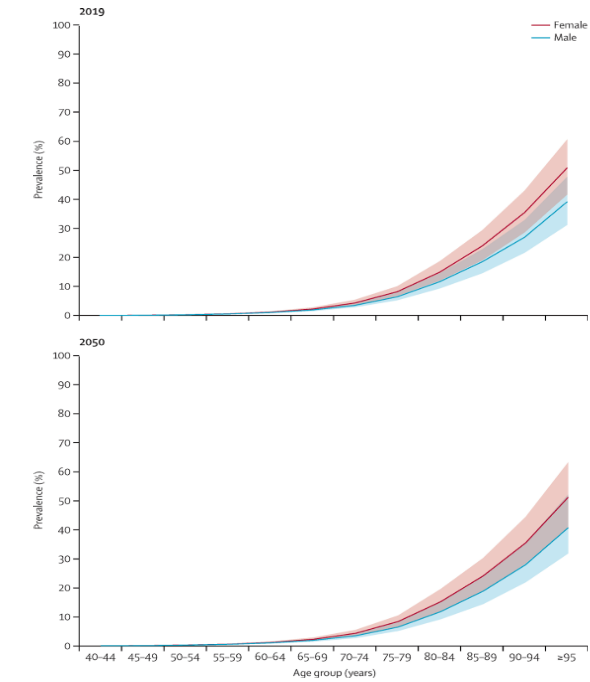
A recently published retrospective cohort study in JAMA Neurology analyzed more than 5.7 million Medicare (U.S.) fee-for-service beneficiaries aged 65 years and older who were newly diagnosed with dementia between 2013 and 2021, with follow-up of up to 8 years. Dementia was identified in participants (58% women) who had been enrolled in Medicare for at least one year, using diagnostic codes from sources such as the International Classification of Diseases, 9th Revision (ICD-9). The primary outcome was all-cause mortality; secondary outcomes included healthcare utilization. Analyses were adjusted for demographic characteristics, comorbidities, and county-level healthcare resources (1).
Study Findings:
- Women with dementia had lower crude one-year mortality compared to men (22% vs 27%) and lower all-cause hospitalization rates (47% vs 51%; P < .001 for both).
- In unadjusted analyses, men had higher one-year mortality risk than women (hazard ratio [HR] 1.30; P < .001), as well as higher risks of all-cause hospitalization (HR 1.13), hospice stay (HR 1.09), hospitalization for neurodegenerative or behavioral disorders (HR 1.24), neuroimaging utilization (HR 1.08), and receipt of physical or occupational therapy (HR 1.07; P < .001 for all). However, men had lower risk for nursing home stay (HR 0.97; P < .001).
- After full adjustment, men still showed higher risks of mortality (adjusted HR [aHR] 1.24), all-cause hospitalization and hospice stay (aHR 1.08 for both), hospitalization for neurodegenerative or behavioral diagnoses (aHR 1.46), and neuroimaging utilization (aHR 1.04; P < .001 for all).
- Men with dementia also spent fewer days in hospice and nursing facilities compared with women (rate ratio [RR] 0.92; P < .001 and RR 0.97; P = .01, respectively).
The study authors concluded that male patients with dementia face higher mortality and greater healthcare utilization—particularly hospitalization—compared to female patients. Strategies aimed at reducing mortality and healthcare use among men with dementia could play an important role in alleviating the overall burden of the disease. Additionally, since dementia prevalence is higher among women, preventive efforts targeting dementia may help achieve population-level health equity regarding gender-based differences in dementia-related mortality.
As part of comprehensive dementia management, effective and optimized treatment plays a crucial role in reducing mortality risk and improving patient health. Vinphaco offers high-quality products containing piracetam—shown to have positive effects on memory improvement—such as KA.NA.CETAM injection (Piracetam 2g) and VINPHACETAM tablets (Piracetam 400mg), contributing to effective and safe management of memory impairment.

References:
- Lusk JB, Ford CB, Soneji S, et al. Sex Differences in Mortality and Health Care Utilization After Dementia Diagnosis. JAMA Neurol. Published online August 11, 2025. doi:10.1001/jamaneurol.2025.2236
- Nichols, E., Steinmetz, J. D., Vollset, S. E., Fukutaki, K., Chalek, J., Abd-Allah, F., … & Liu, X. (2022). Estimation of the global prevalence of dementia in 2019 and forecasted prevalence in 2050: an analysis for the Global Burden of Disease Study 2019. The Lancet Public Health, 7(2), e105-e125.
- https://www.medscape.com/viewarticle/men-dementia-greater-risk-death-hospitalization-2025a1000mif?&icd=login_success_email_match_fpf

 Myanmar
Myanmar